Posture is routinely assessed by a pulmonology hospital as part of a respiratory evaluation, as it can impact breathing and lung function. Posture distortions will limit the amount of air that can enter the lungs, leading to shallow breathing and decreased lung capacity.
As pulmonologists specialize in diagnosing and treating lung and respiratory conditions, assessing posture is a relevant aspect of a comprehensive evaluation to determine the underlying cause of a patient’s respiratory symptoms. Because posture can play a significant role in the management of lung and respiratory conditions, assessing posture as part of a comprehensive evaluation to determine the best course of treatment is increasingly common.

Posture and Respiratory Function
Posture can worsen respiratory function in some lung and respiratory conditions, particularly those that affect the ability to breathe deeply or efficiently. For example:
- Chronic obstructive pulmonary disease (COPD): Poor posture leads to shallow breathing, which reduces lung capacity and makes it harder for patients with COPD to breathe.
- Asthma: Poor posture limits the amount of air that enters the lungs and causes the chest to expand less, making it harder for patients with asthma to breathe.
- Sleep apnea: Poor sleep posture worsens sleep apnea symptoms by narrowing the airway and making it harder to breathe while sleeping.
On the other hand, good strong posture can help improve breathing and lung function in some cases, especially after posture awareness and posture correction exercises patients learn to align their bodies, sitting or standing up straight so that the lungs have enough room to expand and take in more air.

Respiratory Evaluation
The pulmonologist or respiratory therapist performing a posture assessment during a clinical examination, should include observing the patient’s standing and sitting positions, and asking the patient to perform certain movements or breathing exercises. Frequently other diagnostic tools, such as spirometry or chest x-rays, to evaluate lung function and determine if there is a relationship between posture and breathing difficulty are used.
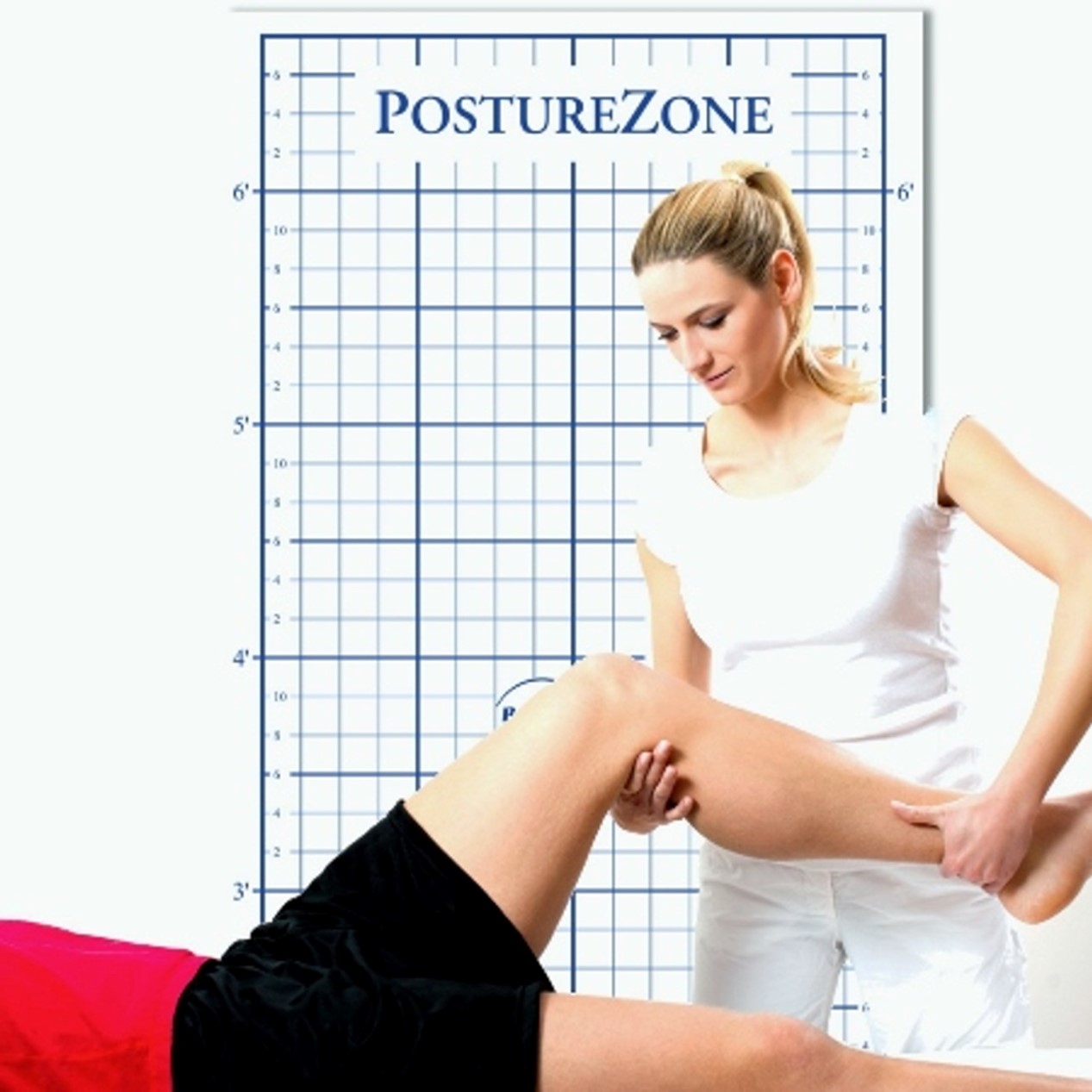
A posture grid is an increasingly popular tool used in the respiratory evaluation. It is a grid-like chart affixed to the wall (wall grid), which is used to quantify and measure various aspects of posture, such as the curvature of the spine and the alignment of the joints. The therapist or doctor will observe the patient from the front, back, and side and compare the patient’s posture to the lines on the posture grid, taking into account various factors such as the patient’s height and body shape. By using a posture grid, the pulmonology / respiratory team can objectively measure and quantify changes in posture over time and determine the relationship between posture and respiratory function.
The evaluation of posture using a posture wall grid is a newer aspect of a comprehensive respiratory evaluation, and the specific posture assessment methods used will depend on the patient’s individual circumstances and symptoms, and the pulmonology hospital or respiratory rehab program.
There have been several studies that have investigated the relationship between posture and pulmonary or respiratory issues. The studies show that poor posture can negatively impact breathing and lung function, particularly in individuals with lung and respiratory conditions.
Effect of Posture on Lung Function
Research studies also show that shallow breathing and reduced lung capacity, which can be the result of slouching or poor posture habits, can make it harder for patients with COPD to breathe and can worsen their symptoms. Other studies have shown that good posture can improve lung function and reduce symptoms in individuals with respiratory conditions.
Recent research has emphasized the interconnection between posture and respiratory function, particularly in clinical settings. A study by Weiniger and Schilaty (2024) introduces the concept of “interoceptive posture awareness and accuracy” (IPA&A), which could have significant implications for respiratory health. While not directly focused on pulmonary function, their work on posture assessment and body awareness aligns with the growing recognition in pulmonology of posture’s impact on breathing. This holistic approach to posture and body awareness could potentially enhance current practices in respiratory evaluation and treatment. By integrating insights from both fields, healthcare professionals might develop more comprehensive strategies for addressing respiratory issues that consider both the mechanical aspects of posture and the patient’s internal awareness of their body positioning.
It’s important to note that more research is needed to determine the role posture plays in increased or diminished lung capacity or ability to breathe deeply when a patient presents with chronic obstructive pulmonary disease (COPD), asthma, pulmonary fibrosis, bronchitis, emphysema, lung cancer, sleep apnea, Interstitial lung disease and cystic fibrosis.
Introducing posture assessments early in care and sharing the results of the posture picture (showing patient in front of the wall grid, AP, PA, Lateral views, sitting and standing) can be a valuable communication and motivational tool for the patient, as well as provide progress documentation for the clinician and respiratory team.
Additional Reading:
- Posture Pictures: Posture Assessments, Screenings (Discusses how to perform a posture assessment)
- Stand Taller Live Longer, Posture and Anti Aging Strategy (Discusses posture exercises)
- Posture Rehab Protocol (Discusses posture correction program for patients with manual and handouts)