The orthotic and pedorthic industry stands at a pivotal moment in its evolution. Certified orthotist and pedorthist demand is projected to grow 17% from 2018 to 2028, while the Prosthetics & Orthotics Market is projected to grow at 6.1% CAGR, reaching $11.24 Billion by 2029. This growth coincides with a technological revolution that’s fundamentally changing how we approach custom orthotic design and manufacturing.
From Static Impressions to Dynamic Data
Traditional orthotic manufacturing has long relied on static foot impressions—plaster casts or foam boxes that capture a single moment in time. While these methods served the industry well for decades, they inherently miss critical information about how patients actually move and function throughout their daily activities.
Traditional orthotic methods rely on static foot impressions, while 3D printing uses dynamic data from volumetric scans and gait analysis. This ensures the orthotic addresses not just the static shape but also the unique movement patterns of the foot. This shift from static to dynamic assessment represents more than just a technological upgrade—it’s a fundamental reimagining of how we understand and address patient needs.

The Power of Precision: Digital Scanning Technology
Modern 3D scanning technology has revolutionized the data collection process. Crafting custom orthotics using 3D printing requires a 3D scanner, CAD software, and a 3D printer with a compatible material. These sophisticated systems capture thousands of data points in seconds, creating detailed digital models that reveal subtleties impossible to detect through traditional casting methods.
The accuracy improvements are remarkable. These digitally manufactured insoles are extremely accurate and ensure 100% repeatability and accuracy. They can even have designs with different levels of stiffness integrated into the prescription ensuring maximum accuracy, durability and comfort. This precision extends beyond just dimensional accuracy—it enables practitioners to incorporate variable density zones, targeted support areas, and graduated flexibility profiles that were previously impossible to achieve.
Comprehensive Patient Assessment: Integrating Traditional and Modern Approaches
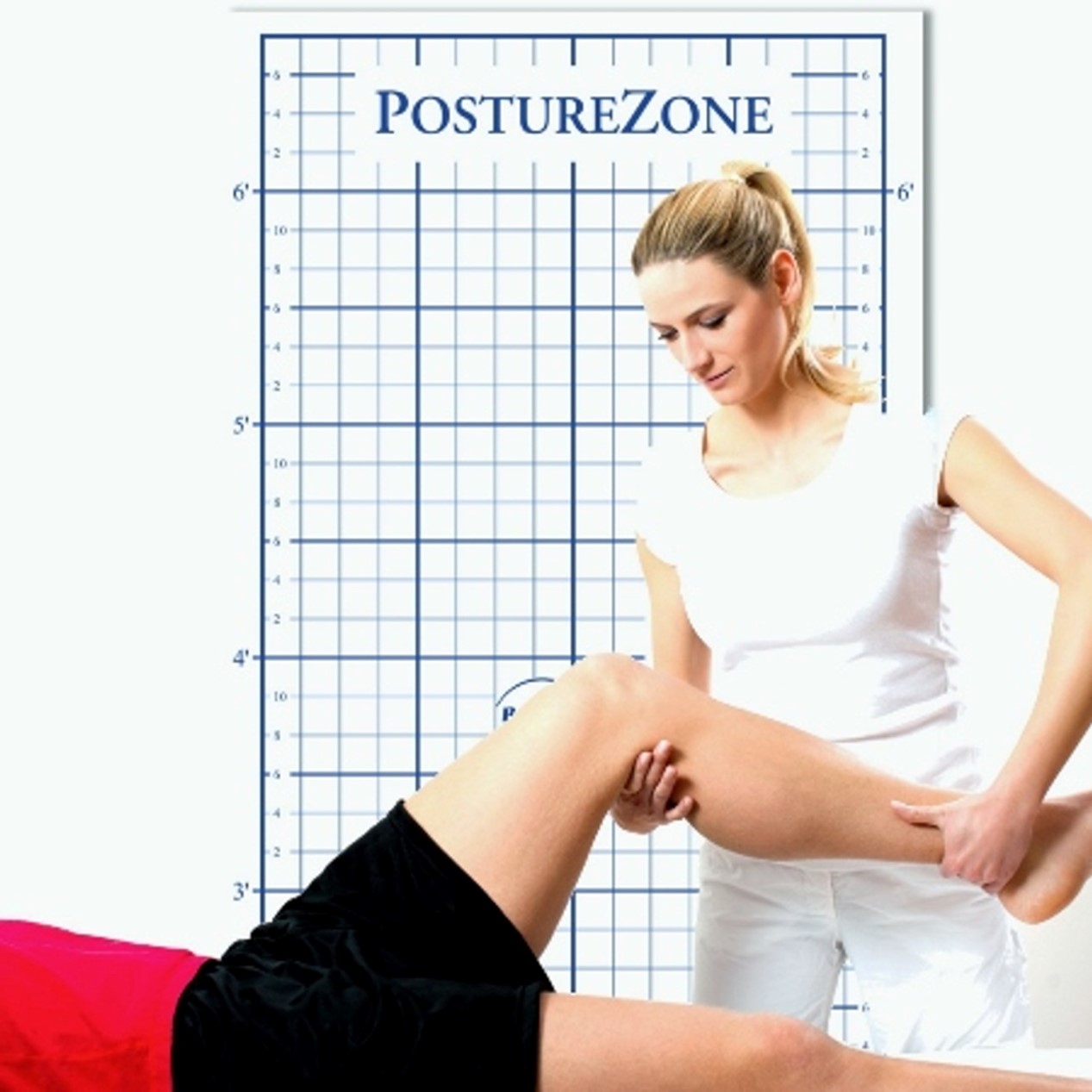
While digital scanning provides unprecedented detail about foot structure and function, comprehensive patient assessment still benefits from established clinical evaluation methods. The posture grid remains an invaluable tool for systematic postural analysis, allowing practitioners to objectively document spinal alignment, pelvic positioning, and weight distribution patterns that directly influence lower extremity function.
When practitioners combine traditional posture grid analysis with modern 3D scanning data, they create a more complete clinical picture. The posture grid helps identify proximal influences on foot function—such as pelvic obliquity or spinal asymmetries—while digital scanning captures the precise structural adaptations that have occurred distally. This integrated approach transforms both subjective postural observations and detailed anatomical measurements into objective, measurable data that guides comprehensive treatment planning.
The synergy between posture grid assessment and digital foot scanning enables practitioners to address not just local foot pathology, but also the broader biomechanical chain that influences patient symptoms and functional limitations.

Manufacturing Revolution: Speed Meets Customization
The manufacturing benefits of 3D printing technology are equally impressive. A pair of custom foot orthotics can be printed in less than 5 hours by using one printer. For a busy clinic, two printers can be used to speed up the production. For re-makes, it only take 2 hours to re-print 1 orthotic device. This dramatic reduction in production time doesn’t just improve patient satisfaction—it fundamentally changes practice economics and workflow management.
The repeatability factor cannot be overstated. Once a digital design is perfected, identical replacements can be produced indefinitely without degradation in quality or accuracy. This addresses one of the most persistent challenges in traditional orthotic manufacturing: ensuring consistent quality across multiple pairs or replacement devices.
Evidence-Based Outcomes
Research continues to validate the clinical advantages of these advanced manufacturing techniques. Pedorthists and orthotists achieved greater maximal peak pressure reductions calculated over the whole forefoot than podiatrists: 960, 1020 and 750 kPa, respectively. While this study predates many current technological advances, it demonstrates the specialized expertise that pedorthists and orthotists bring to orthotic design and manufacturing.
Integration Challenges and Solutions
The transition to digital workflows isn’t without challenges. Many practices struggle with the initial investment in equipment, software training, and workflow modifications. However, the long-term benefits—improved patient outcomes, reduced remake rates, enhanced practice efficiency, and competitive advantages—typically justify the investment within the first year of implementation.
Successful integration requires a systematic approach. Practices must consider not just the hardware and software components, but also staff training, quality control protocols, and patient communication strategies. The most successful implementations involve gradual adoption, starting with straightforward cases and progressively expanding to more complex prescriptions as expertise develops.

The Future Landscape
Looking ahead, the integration of artificial intelligence, machine learning algorithms, and predictive modeling promises to further enhance orthotic design capabilities. These technologies will help practitioners identify optimal design parameters based on patient-specific data, predict long-term outcomes, and continuously refine treatment approaches based on aggregated patient responses.
The convergence of digital scanning, advanced manufacturing, and data analytics is creating unprecedented opportunities for precision medicine in orthotic care. Practitioners who embrace these technologies position themselves at the forefront of patient care while building more efficient, profitable practices.
Practical Implementation Steps
For practices considering the transition to digital workflows, the path forward involves several key considerations. Begin with a thorough assessment of current patient volume, remake rates, and workflow bottlenecks. Evaluate different scanning and printing solutions based on your specific practice needs, considering factors like patient demographics, prescription complexity, and growth projections.
Invest in comprehensive staff training and establish clear quality control protocols. Develop patient communication strategies that highlight the benefits of advanced technology while maintaining the personal touch that defines excellent patient care. Most importantly, approach implementation as an iterative process, allowing time for adjustment and optimization as your team gains experience with new tools and workflows.
The digital revolution in orthotic manufacturing represents more than just technological advancement—it’s an opportunity to elevate patient care, improve practice efficiency, and position your services at the forefront of modern healthcare delivery. The question isn’t whether these technologies will become standard practice, but how quickly forward-thinking practitioners will adopt them to serve their patients better.