Elevating Oral-Systemic Care Through Posture Analysis
As speech therapists, speech-language pathologists and orofacial myofunctional therapists treating oral and craniofacial dysfunction, you understand the vital links between the head, neck, breathing and body alignment. Integrating posture assessments into your practice can provide immense clinical value and enhanced outcomes.

Why Add Posture Analysis to Your Practice?
At minimum, conduct quick posture screens during initial evaluations and discharge. Comprehensive postural analysis every 4-8 weeks will allow you to track changes over therapy. Here are some key benefits:
- Identify anatomical and biomechanical factors affecting oral rest posture, swallowing, and respiration
- Recognize postural patterns associated with bruxism, tongue thrust, open bite and crossbite
- Monitor improvements in head and neck positioning in patients with TMD or cervical instability
- Educate patients on postural habits that may exacerbate TMJ dysfunction or tongue tie
- Demonstrate progress that motivates patients with dysphagia, speech delays or myofunctional disorders
- Determine needs for additional therapy or medical referrals
- Quantify outcomes that highlight the value of your specialized care
How to Integrate Posture Screenings
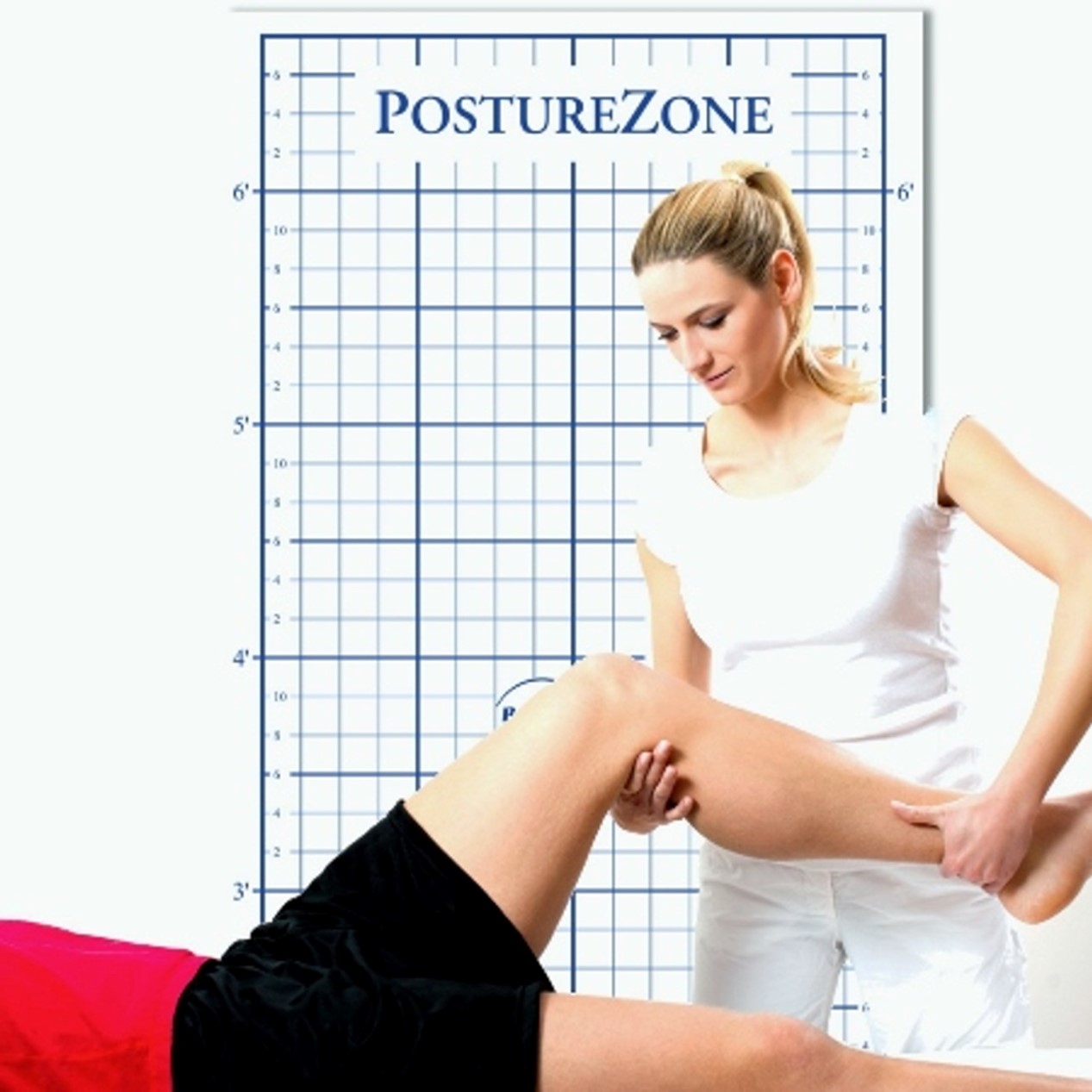
Use a wall-mounted posture grid or door-mounted posture grid during assessments. These are the most accurate and durable options especially for practices working with children. Capture comparative photos from multiple angles as patients stand naturally.
Start with facing forward, facing to the right or left, and facing backward. You might also take a front view and side view of the patient’s sitting posture. Analyze for forward neck, rounded shoulders, uneven weight distribution and more.
Patient Education and Progress Tracking
Guide patients through results, explaining the postural factors impacting their specific oral conditions. Patients and parents appreciate this clinical insight.
Adding posture analysis takes little time but yields significant rewards. You gain comprehensive insights, demonstrate expanded value, and reinforce your oral-systemic expertise. With routine consistency, it’s a best practice that elevates patient care.
You might have an interest in reading about this study that evaluated postural changes using posturography testing in patients with dysfunctional dysphonia before and after speech rehabilitation, in order to analyze variations in their balance and stability resulting from therapy.
The study investigated the relationship between voice issues and posture in patients with dysfunctional dysphonia. The researchers evaluated postural changes in 40 subjects before and after speech rehabilitation treatment.
They used posturography testing to analyze variables related to the patients’ balance and stability while standing. At baseline, patients showed alterations in parameters like the area and speed of their movement during the test.
After undergoing speech therapy, all of the postural variables improved, especially in measures of variability in their movement. This indicates they had better control and stability. Their overall center of pressure also shifted backwards after rehabilitation.
These results show that for patients with voice disorders like dysfunctional dysphonia, speech therapy can help improve awareness of body positioning and postural control. The posturography testing was able to quantify those postural changes before and after treatment.
In summary, the study demonstrates a connection between voice and posture. It suggests that speech rehabilitation in patients with voice disorders can have secondary benefits on their posture and balance. Testing posture provided an objective way to measure those therapeutic improvements.